From Nappy Rash to Mystery Rashes:
Demystifying and Treating Skin Conditions in Babies and Children
Rashes are very common in babies and children and a topic many parents worry about. Most rashes are harmless and will go away on their own. Below are some of the common rashes with information on what to look out for and the treatment.
NAPPY RASH
Nappy rash is a very common skin condition in children under two. It’s caused by the skin coming into contact with urine (wee) and faeces (poo) in the nappy. Mild cases are usually painless. But, severe nappy rash can hurt and upset babies.
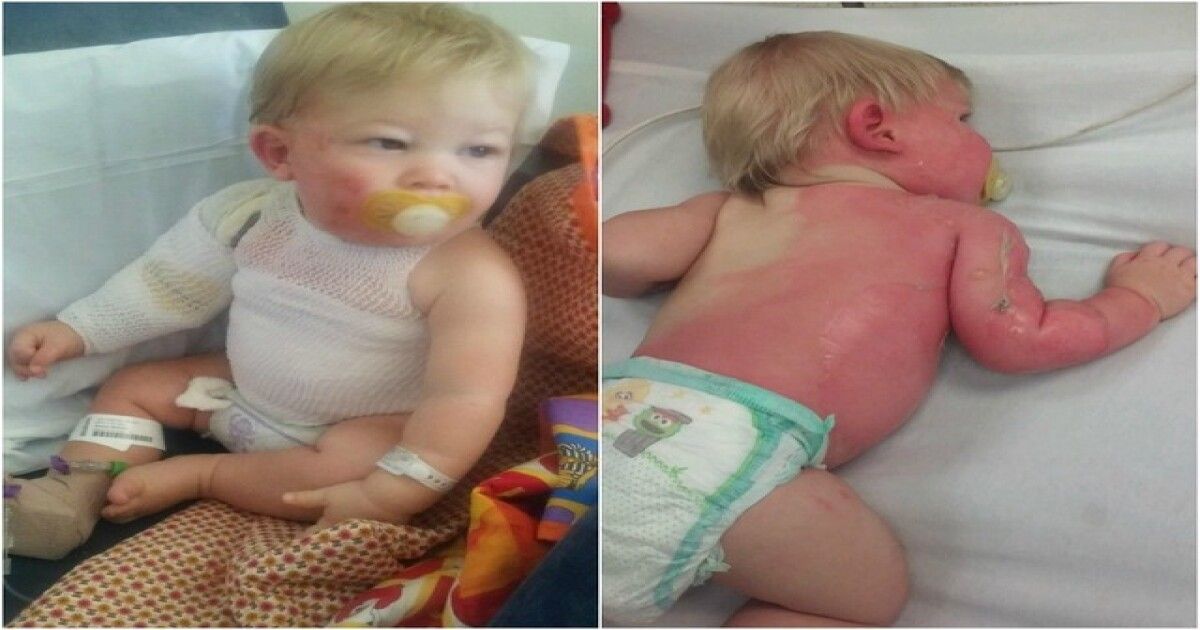
The main symptom of nappy rash is red, raw skin in the nappy area. The rash might spread to the baby’s tummy or up their back. The skin might be raised or swollen.
If your baby has nappy rash there are some things you can do to help manage the condition:
- try to leave your baby’s nappy off whenever possible. This will keep your baby’s skin dry and away from any contact with wee or poo. Try laying your baby on a towel during tummy time or any floor play. You should always watch that they have not wet or soiled the towel so that they are not left on a damp towel
- change your baby’s nappy regularly
- only use warm water to clean the rash area
- avoid soaps and perfumed baby wipes as these can irritate the skin
- use soft towels or cotton wool when drying the skin, and dab the area gently
- apply a barrier cream after changing every nappy. Products containing zinc cream, zinc oxide ointment and petroleum jelly are all suitable. You can also ask your pharmacist about nappy rash creams
- do not use talcum powder or antiseptics
See a doctor if:
- the rash doesn’t clear up in one week
- there are blisters, crusts or pimples
- your baby has a fever
- the rash is spreading
- your baby is very upset
- if you have a son, the end of his penis is red and swollen or has a scab
IMPETIGO (SCHOOL SORES)
Impetigo ‘school sores’ is a very common skin infection that causes sores and blisters. It affects mainly children.
Impetigo is contagious and can be very dangerous for newborn babies. It’s important to keep children with impetigo away from babies. They should not go to school or childcare until treatment starts.
Impetigo causes sores on the skin. These can be in the form of blisters that grow quickly, then burst and leave a moist area with a brown crust at the edge. The blisters can be large (several centimetres across) and quite itchy. Sometimes the sores have a thick, soft, yellow crust with a moist red area underneath.
The sores appear 1 to 3 days after exposure to the infection. They are contagious as long as there is fluid weeping from them. They are no longer contagious when the sores have scabbed over. Or, it's 24 hours after they start antibiotic treatment.
If you have impetigo there are some things you can do to help manage the condition.
- Wash sores with salty water (1 teaspoon of table salt dissolved in a cup of hot water and left to cool) 2 to 3 times a day. Pat dry, using a new towel each time, then apply the antibiotic cream as prescribed.
- Cover sores with waterproof dressings that do not have any holes. Throw all dressings in the bin straight after you take them off and wash your hands.
- The affected area can become irritable and itchy. It is important to not scratch it because it can make the impetigo spread and get worse.
See a doctor:
Doctors usually prescribe antibiotics as a cream, ointment, tablets, or syrup. The form depends on the severity of the condition. Always complete the full course of treatment.
HIVES
Hives (urticaria) are common skin rashes. They have one or many wheals (lumps) of reddened, raised, and itching skin. The wheals can vary in size, from relatively small to as large as a dinner plate. The wheals may be circular, oval or ring shaped.
Hives can affect any part of the body, but is common on the torso, throat, arms and legs. The wheals appear in clusters. One cluster gets worse as another gets better. Most wheals disappear without a trace within a few hours, only to be replaced by a new one elsewhere on the skin. Wheals that stay in the same spot for more than 24 hours may state a different disorder.
In 80% of cases the cause of hives is unknown. Some factors known to cause hives include:
- medication – such as antibiotics, aspirin and codeine
- allergic reactions to foods
- some food additives
- infections – including bacterial or viral
- respiratory infections (particularly in young children)
- contact with plants or animals
- heat
- cold temperatures
- exercise and sweating
- bee and wasp stings
If a trigger is identified and it is possible to avoid that trigger, then the hives will resolve. Where no trigger is found, or the trigger cannot be avoided, treatment may include:
- Avoid things that make the condition worse. These include aspirin, codeine, sunshine, heat, and hot showers.
- antihistamines – some people need 2, 3 or even 4 tablets a day to control hives. These are available from pharmacies without prescription. Some antihistamines cause drowsiness.
For more information: https://www.rch.org.au/kidsinfo/fact_sheets/Rashes/
Disclaimer: The health information provided is for informational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of a qualified healthcare provider with any questions you may have regarding a medical condition.

Baby First Aid QLD is a business for good that is on a mission to ensure all parents and carers have access to quality skills in first aid to apply if their child is sick, injured or in an emergency situation.
We provide our courses across Queensland, so would respectfully like to acknowledge the traditional owners of our land, past, present and emerging. We are committed to learning and understanding the truth of our First Nations people and sharing this truth. We would like to acknowledge the traditional owners of the land that we work, play and care for our families on.
Baby First Aid QLD would also like to extend our respect to the LBGTQIA+ community and show our commitment to being an inclusive enterprise. We stand by strong principles and take pride in living by these.
The creation of this website was made possible through grant funding from the Queensland Government via the Social Enterprise Grant from the Department of Education, Small Business and Training (DESBT).

Website Disclaimer
The information provided by Baby First Aid Qld is for general informational purposes only. All information on the Site is provided in good faith, however we make no representation or warranty of any kind, express or implied, regarding the accuracy, adequacy, validity, reliability, availability or completeness of any information on the Site. Under no circumstance shall we have any liability to you for any loss or damage of any kind incurred as a result of the use of the Site or reliance on any information provided on the Site. Your use of the Site and your reliance on any information on the Site is solely at your own risk.